
Introduction
Mental health care for youth, particularly in early childhood, is a pressing issue. Recent studies reveal that one in five children aged 3 to 17 in the US has a mental disorder. The COVID-19 pandemic has further exacerbated these conditions, highlighting the urgent need for effective mental health services. A recent article explored the prevalence of mental disorders among young children and the barriers they face in accessing necessary care. Their focus was on improving mental health services for youth, a critical aspect of value-based healthcare.
Understanding Early Childhood Mental Disorders
Mental disorders in early childhood can significantly impact a child’s development and well-being. These disorders often manifest as anxiety, depression, ADHD, and behavioural issues. The prevalence of these conditions has increased over the years, with 19% of children in early childhood having been diagnosed with a mental disorder. This represents a 9% relative increase since 2016. Early intervention is crucial as it can prevent long-term cognitive, emotional, and social challenges.
Barriers to Accessing Mental Health Services
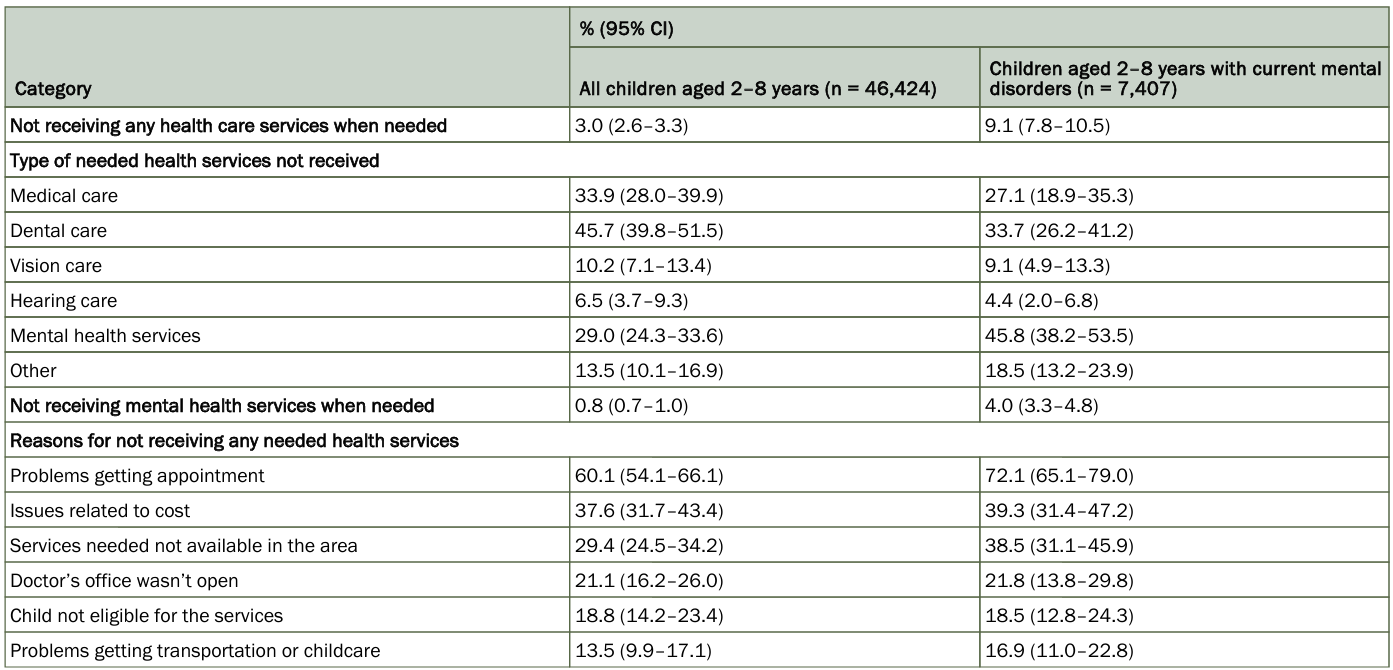
Despite the availability of evidence-based treatments, many children with mental disorders do not receive the necessary care. In this study, 9.1% of children with current mental disorders did not receive any needed health services. The primary barriers include lack of access to healthcare services and negative experiences with healthcare providers. Moreover, health insurance often fails to cover the needed services, making it difficult for families to obtain the required care.
Improving Access to Mental Health Services
Addressing the barriers to mental health services involves multiple strategies. Firstly, enhancing the availability of mental health services is essential. This includes expanding healthcare coverage to ensure all children have access to the necessary services. Secondly, improving the patient experience with healthcare providers can foster trust and encourage parents to seek help for their children. Lastly, creating patient-centred communication strategies can help families understand mental health needs and treatment options.
The Role of Value-Based Healthcare
Value-based healthcare focuses on providing high-quality care that improves patient outcomes. In the context of mental health care for youth, this means prioritising early intervention and ensuring access to necessary services. By integrating value-based healthcare principles, we can improve the mental well-being of children and reduce the long-term impact of mental disorders.
Conclusion
The increasing prevalence of mental disorders among young children emphasises the need for improved mental health services. By addressing the barriers to care and adopting value-based healthcare principles, we can enhance the mental well-being of our youth. This requires a collaborative effort from healthcare providers, policymakers, and the community. Together, we can ensure that all children have access to the mental health services they need.
